Basal Cell Carcinoma
Basal Cell Carcinoma
- About
- Treatment
- FAQs
About
Basal Cell Carcinoma
This is the most common type of skin cancer. It most often appears on skin exposed to the sun, such as the face, scalp, neck, hands, and arms, but can appear on any part of the body.
BCC may never metastasize, but they can grow deep and wide, affecting surrounding tissue and structures. This is especially concerning on the face where such alteration can affect the eyes and ears, and be cosmetically difficult to handle.
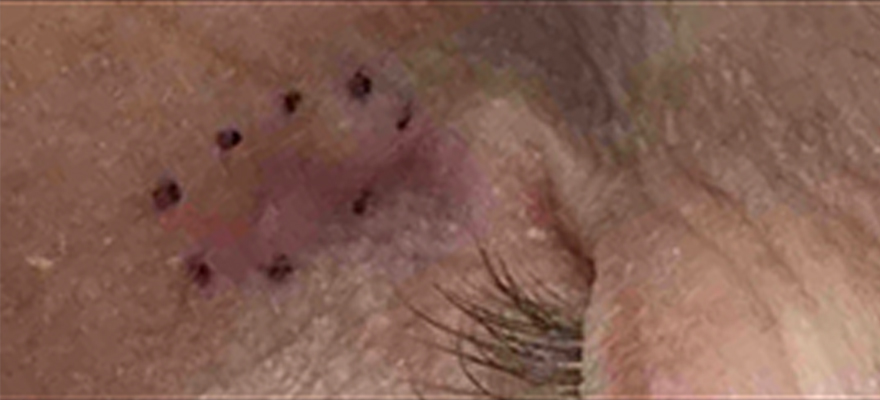
BCC often grows slowly. It may look like a:
- Reddish patch of dry skin that won’t heal
- Flesh-colored (or pink, red, or brown) pearl-shaped lump with visible blood vessels
- Pimple that just won’t clear
- Sore that bleeds, heals, and then returns
- Scar that feels waxy — may be skin-colored, white, or yellow
- Group of slow-growing, shiny pink or red growths that look like sores, often scaly and bleed easily
- Flat or sunken growth — feels hard, may be white or yellow
Risk Factors
People of all skin colors can get BCC, although it is much more common in light-skinned people. The sun’s ultraviolet (UV) rays damage your skin. Your everyday activities expose you to UV rays, such as going outdoors during the day without sun protection or when you drive your car or sit near your office window. Additionally, tanning beds emit dangerous UV rays and their use is associated with developing BCC and other types of skin cancers.
Your risk of developing skin cancer increases as this damage accumulates. There are some people though who have a higher risk of getting BCC. For example, the risk increases with age. The older you are, the longer you have been exposed to the sun’s UV rays. People also may have a higher risk of developing BCC when they have:
- Pale, light-colored or freckled skin
- Blonde or red hair
- Blue, green, or gray eyes
- A family history of skin cancer
- A weakened immune system or are taking medicine that suppresses the immune system
- Used tanning beds or other indoor tanning devices
Diagnosis
To diagnose BCC, a dermatologist performs a skin biopsy. This is the only way to confirm a diagnosis of skin cancer, including BCC. Your dermatologist can perform a biopsy using local anesthesia during an office visit.
Your dermatologist will biopsy all or a representative sample of the growth depending on its size and location on your body. This tissue will be sent to a pathologist to evaluate under the microscope and determine the diagnosis.
If the diagnosis is BCC, your dermatologist will consider many factors to determine the best treatment for you, including where the BCC appears on your body, the size and features of the BCC, and your overall health.
*Source:
American Academy of DermatologyTreatment
Treatment
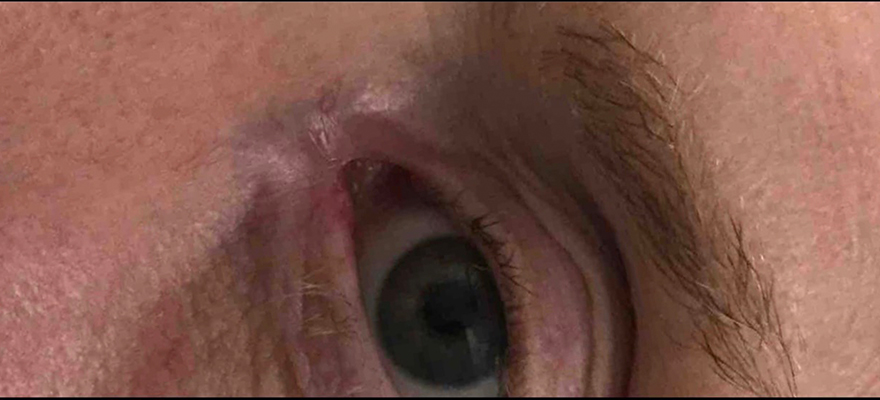
When detected early and treated properly, the prognosis for BCC is excellent. Treatment cures most BCCs. Treatment for BCC involves having one or more of the following.
There are many effective treatments. A dermatologist selects treatment after considering the following: the type of BCC, where it appears on the body, a patient’s overall health. After considering this, one or a combination of the following treatment options may be recommended.
- Surgical treatment: Surgical removal can be done in a dermatologist’s office under local anesthesia using one of the following techniques. A small amount of normal skin is also removed as skin cancer cells can microscopically involve normal looking skin.
- Excision: The lesion and a small amount of normal-looking skin (margins) surrounding the skin cancer are cut. What is removed is sent, like the initial biopsy, to a pathologist for microscopic examination to ensure all of the margins are clear of the skin cancer. Stitches are used for wound closure.
- Mohs surgery: A dermatologist who has completed additional training in Mohs surgery performs this procedure. The skin cancer and a much smaller margin of normal skin is removed and checked immediately in the office. If any of the margins are still involved in the skin cancer, that specific area of involved skin is taken and rechecked. This occurs until all margins are clear. Once this is achieved, the surgeon may use different techniques including flaps or grafts, to close the skin together.
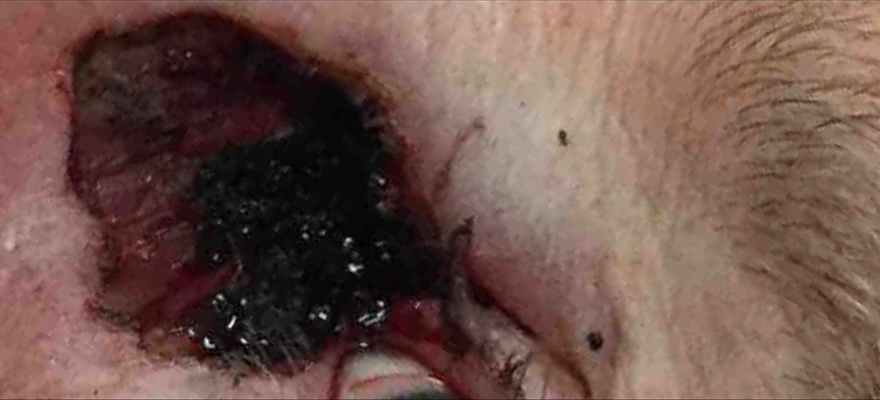
- Curettage and electrodesiccationThis surgical procedure may be used to treat shallow basal cell and squamous cell skin cancers. It involves scraping the tumor with a curette (a circular blade) followed by gentle cauterization (burning) of the site. This scraping and cauterizing process is typically repeated 3 times. The wound may heal without stitches.
- Radiation therapy: Radiation may be used to treat older adults who have a large skin cancer, skin cancers that cover a large area, or a skin cancer that is difficult to surgically treat. Radiation therapy gradually reduces the cancer cells through repeted exposure to radiation. A patient may receive 15 to 30 treatments. Many years after a person is exposed to radiation, there is a risk of new skin cancers developing in the treated skin.
- Topical Immuno- or chemotherapy: There are creams that a patient applies to the skin as directed by the dermatologist that can help the body’s own immune system fight the cancer, or intentionally damage the dangerous cancer cells.
- Pills: In the very rare incidence that BCC spreads to other parts of the body, or in the case of a BCC that has become very large and is not amenable to traditional surgery or radiation, an oral medication may be an option.
What we do
Products- All Sunscreens
- Heliocare
Procedures
- Full Body Skin Examinations
- Biopsies to confirm the diagnosis
- Electrodesiccation & curettage
- Excisions
Download these treatment information documents:
Wound Care Instructions after Biopsy and ED&CPost-Excision Wound Care Instructions
FAQs
If I have BCC, am I at greater risk of developing other skin cancers?
Yes. Studies show that people who have one skin cancer are at greater risk of developing another skin cancer. Perform regular skin self-examinations, and protect your skin every day. Be sure to keep all appointments with your dermatologist, and make an immediate appointment if you notice anything changing, itching, or bleeding on your skin.
Can anyone get BCC?
Yes. People of all skin colors can get BCC, although it is much more common in light-skinned people.
Are tanning beds ever safe?
No. Never use a tanning bed. UV light from tanning beds can cause skin cancer and wrinkling. If you want to look tan, consider using a self-tanning product. Remember that even when using one of these products, you need to use sunscreen.
What does SPF mean?
SPF stands for “Sun Protection Factor.” It is a measure of how well the sunscreen protects you from harmful UV rays from the sun. Sunscreen must be re-applied every two to three hours, even if it has a high SPF number. Adults and children should always wear at least SPF 30.